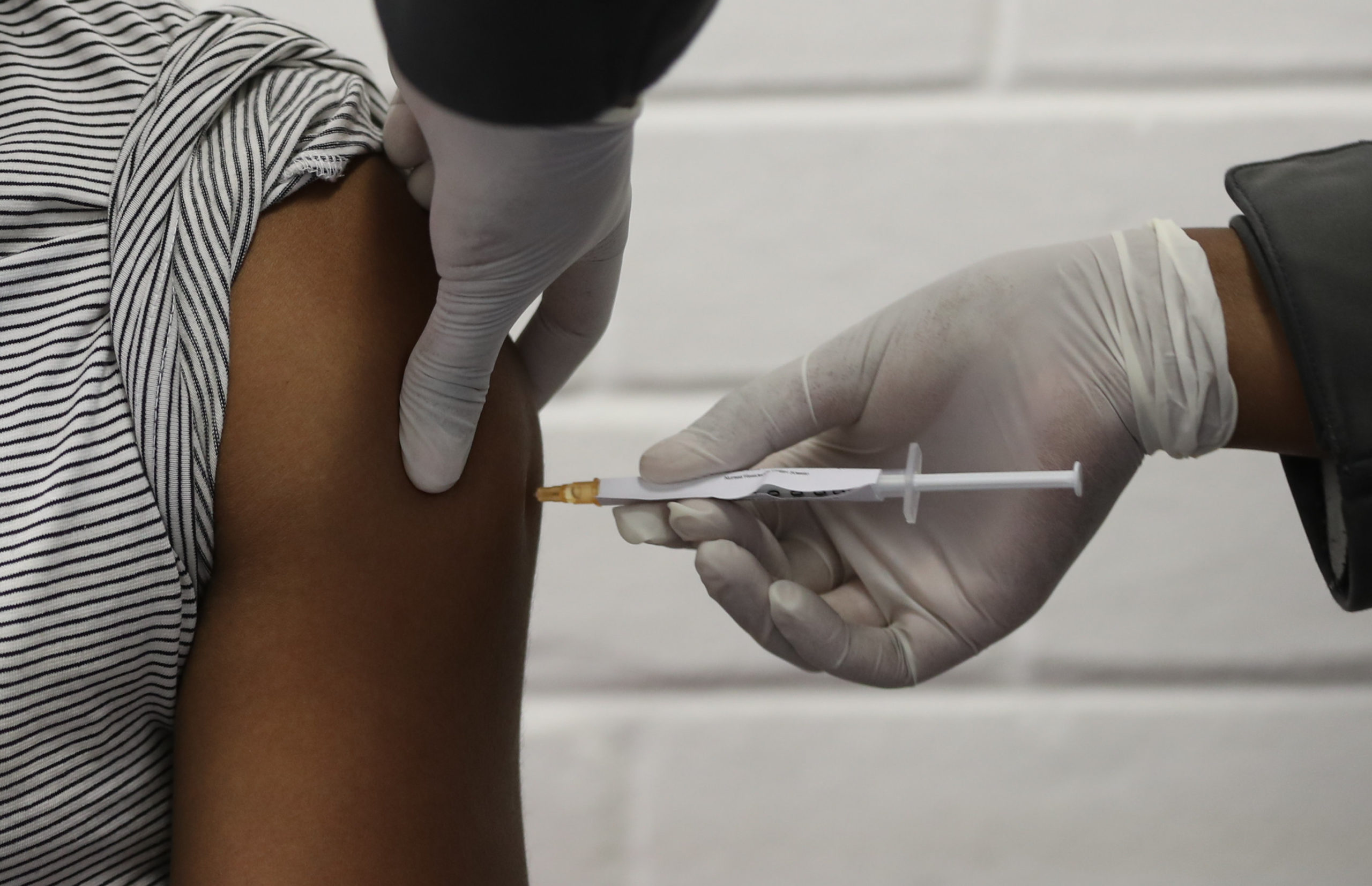
Scientists are optimistic theyll find a coronavirus vaccine. The bad news? They might need to vaccinate the entire globe every year.
With most countries banking on a vaccine as their exit strategy, the ideal scenario is finding a single shot that inoculates people against the deadly virus for the rest of their lives. In reality, regular immunizations could be just as likely based on experiences with the flu, measles and other infectious diseases.
One of the leading vaccine candidates is from the University of Oxford and AstraZeneca, which could be deployed as early as October. However, the head of the pharma company estimated that itll provide immunity against COVID-19 for only up to a year.
If thats the case, the world might be banking on a coronavirus vaccine that requires billions of doses to be doled out annually. “Until we know what level of immune response is needed for protection, we dont [know] whether the immunity we see at one year will be sufficient,” said Sarah Gilbert, leader of the University of Oxford team.
Researchers still understand very little about the coronavirus that has infected millions and killed more than 500,000. The fact that it appears to mutate far more slowly than the flu offers at least one positive sign.
“I dont think its all doom and gloom,” however, “theres still a lot to be learned about the duration of immunity” — Ultan Power, a virology professor at Queens University in Belfast
“Its not like flu that changes its coat all the time and keeps coming back in different versions,” said Gilbert. “The prospects for generating a vaccine against the coronavirus are very good.”
But theres also cause for worry. “We never had a vaccine for [a] coronavirus,” the World Health Organizations Director General Tedros Adhanom Ghebreyesus told the European Parliaments health committee last week. “It would be the first one, and having the first of anything is difficult.”
Other coronaviruses have shown varying lengths of natural immunities. Most people who contracted the coronaviruses that cause SARS and MERS, for example, had immunity up to a year or two — but in some cases it lasted up to a decade.
The risk is that the newest virus could turn out to be more like its cousins that cause the common cold, which are endemic in humans and can reinfect every six months.
“I dont think its all doom and gloom,” Ultan Power, a virology professor at Queens University in Belfast, told a recent hearing in the U.K.s House of Lords. However, “theres still a lot to be learned about the duration of immunity.”
Immunity gamble
Vaccine developers need to prompt the perfect cocktail of immune responses to protect people against a pathogen.
In the bodys natural response system, antibodies — some of which act as virus neutralizers — are produced and directed by a type of white blood cell called B cells. The immune system also deploys various types of T cells, including those that help B cells and others that destroy parts of the body infected by the virus at a microscopic level.
The problem is that vaccine developers dont know which combination they need to produce immunity against the coronavirus, or how long that will offer protection. “For each disease that we want to make a vaccine against, we need to understand what we need the immune system to do to control that disease,” Gilbert said.
One potential pitfall is that there can be key differences between the immunity acquired naturally from having the virus and from getting a vaccine.
With measles, getting the virus once produces a low number of neutralizing antibodies that produce lifelong immunity. The vaccine, however, doesnt produce as strong of a reaction, so people are required to get booster shots.

World Health Organization Director General Tedros Adhanom Ghebreyesus | Fabrice Coffrini/AFP via Getty Images
Another question is whether a strong antibody response is a good thing. There are positive signs that COVID-19 triggers the development of a decent amount of neutralizing antibodies, Power said in an interview.
But there appears to be a correlation between the severity of the disease and the severity of the immune response, which raises questions about whether the immune response actually plays a role in worsening the disease.
In this scenario, the body produces non-neutralizing antibodies that bind to the pathogen and allow the virus to get further into the body.
That reaction was a key reason why, in 2017, the Philippines stopped using a once-promising vaccine that protected against dengue. The vaccine produced immunity from one strain of the virus but sometimes produced too many non-neutralizing antibodies to other strains. This made the disease worse when people were reinfected with a different strain of the virus.
Different from the flu
One thing thats certain is the coronavirus isnt mutating as quickly as the flu.
But this might be because the virus hasnt experienced much immunological pressure yet, Power said. It “remains to be seen” whether itll mutate faster once a large proportion of the population has become immune, he said.
The takeaway is that even if researchers find a successful vaccine against coronavirus, the entire globe would need to be re-vaccinated continually if it doesnt produce long-term immunity.
The coronavirus so far is acting more like human respiratory syncytial virus (RSV), the leading cause of severe lower respiratory infections in children. RSV doesnt mutate very often compared with influenza, but it can cause repeat infections in humans. Theres also no vaccine against it.
Power said he suspects coronavirus will be similar to RSV by failing to create a very strong immune response the first time in humans, which “allows the virus to come back and infect more people.”
What researchers dont understand well about RSV, and potentially about the coronavirus, is what those viruses do to the immune system that means the body fails to build a long-term defense. “That obviously has consequences for the duration of protective immune responses with vaccines,” Power said.
The takeaway is that even if researchers find a successful vaccine against coronavirus, the entire globe would need to be re-vaccinated continually if it doesnt produce long-term immunity.
Its not unheard of to vaccinate the whole globe every year — thats essentially whats tried for influenza. Because the flu mutates so quickly, researchers attempt to predict the virus strains that they expect will be most widespread twice a year.
But vaccination rates for the flu are low. In 2017, Eurostat reportRead More – Source
[contf]
[contfnew]

politico
[contfnewc]
[contfnewc]